BIRTH SERVICES
Birth Options | Part Five: Hospital Policies
If you’ve chosen to birth your baby in a hospital like the majority of women in America, you’ll want to be sure you’re aware of the hospital policies that may affect the way you can labor. The best way to learn more about your specific hospital policies is to talk to your OB or midwife and take a hospital tour as early as possible. Having an idea of what the policies are will help you to create your birth plan and know what questions to ask your care provider. I think it’s important to understand that nothing is 100% required if you aren’t comfortable with it. This is your body, your baby, and your birth. That said, make sure to do your research if you plan to decline anything.

I’ll list a few common hospital policies below with a short description, but as mentioned about, talking to your OB will give you the best idea of what your local hospital does.
- No eating or drinking during labor
Many hospitals have a policy known as “NPO” or “nil per os” which is latin for “nothing by mouth.” These policies are based on old data that suggests that women needing anesthesia or cesareans could inhale stomach contents and suffocate if they’d been allowed to eat or drink during labor. The study was conducted during a time when anesthesia looked very different than it does today but many hospitals continue to keep the policy. You can read more about the history and evidence on NPO HERE.
- No water births
There are many hospitals that offer tubs or showers for laboring moms, which can be a great way to relieve pressure or pain during labor, but it is much more rare to find a hospital that will allow you to actually birth your baby in the water. Once you reach the point of pushing, your care provider may require that you move to the bed to birth your baby there. Be sure to ask about water birth if you are hoping to have that option in a hospital. You can read more about the evidence on water birth HERE.
- Pushing position options
Something that can significantly affect the way you experience your birth is whether or not you are allowed to push in positions other than the “lithotomy” position (lying on your back with feet in stirrups). Often this is the only position we’ve been exposed to and many women may not know their options. Additionally, if you have an epidural, you may think that you can only push on your back, but oftentimes care providers can help you to move into a more effective pushing position so be sure to ask about this! HERE is a great article about the evidence on birthing positions.

- IV fluids required
Many hospitals will require you to have IV fluids upon admittance. As everything that is done to your body is, this is something you can decline. Some women choose to decline IV fluids because they are able to drink water and stay hydrated orally. IV fluids in *large* amounts have been known to make breastfeeding harder and to create swelling in mom and baby. HERE is an article about IV fluids during labor. HERE are some real stories from moms who have had IV fluids during labor.
- Fetal Monitoring
Depending where you’re giving birth, there are lots of different types of fetal monitoring. If you’re unfamiliar with this term, it basically is referring to monitoring the baby’s heartbeat during labor. In a hospital, continuous fetal monitoring (CFM) is often the standard, but you should be able to talk to your care provider about other options as long as you are not using an epidural or Pitocin to augment labor. The most popular reason for opting out of CFM is that mom wants to be able to move freely in order to help labor progress and baby move into position for birth. HERE is a fantastic article on all of your fetal monitoring options!
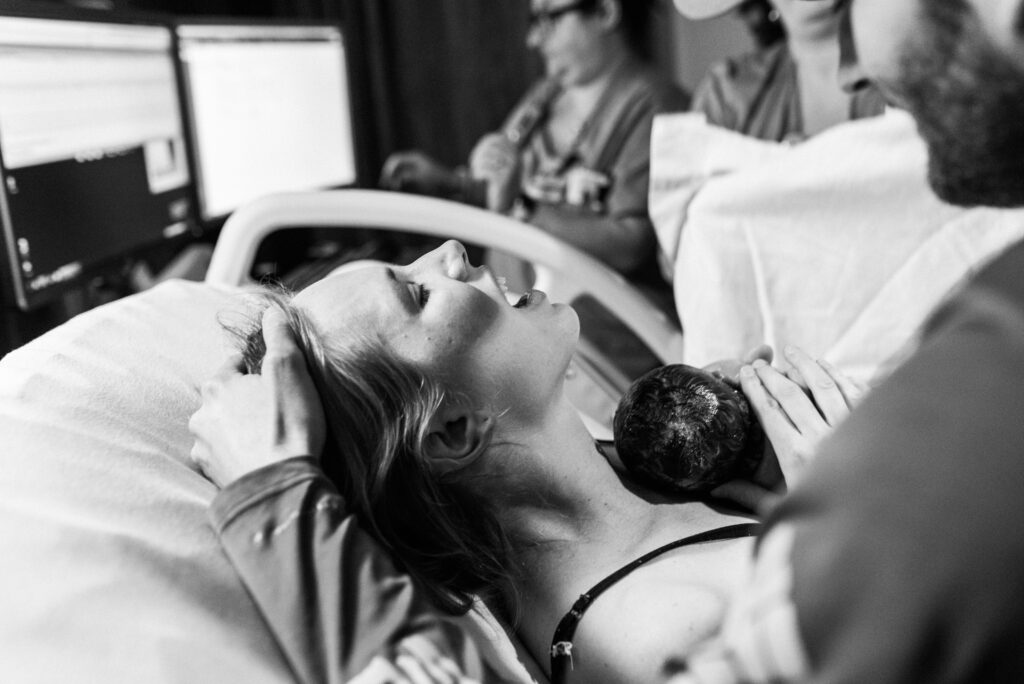
- Delayed cord clamping
After baby is born, many care providers have adopted the practice of clamping and cutting the umbilical cord immediately (within seconds). But there is some research that suggests that all newborns will benefit from delaying the cord clamping and cutting by 1-3 minutes (many midwives suggest waiting until the cord is done pumping blood). Delaying clamping leads to increased hemoglobin levels and iron stores and is especially important for preterm infants. Here are a few articles on the subject: World Health Organization, American College of Obstetrics and Gynecology, Academic OB/GYN.
- Immediate skin-to-skin
Immediate skin-to-skin with baby after birth is definitely becoming a more popular practice at many hospitals, but it’s not a guarantee. Talk to your care provider if this is something you’re interested in! Immediate skin-to-skin contact is associated with better breastfeeding outcomes, more regulated temperatures in newborns, and a more immediate bonding experience. You can learn more about the benefits HERE.
- Delayed newborn bathing
It used to be standard practice to bathe baby right away after birth. Now it’s more common to wait about 24 hours and give baby a bath while still at the hospital, but many mothers are opting to wait until they get home to bathe their babies. There are benefits to not washing off the baby’s vernix (even if there is very little on baby) so the recommendation is to wait a minimum of 8-24 hours. Read more about delayed newborn bathing HERE.
- Cesarean options
I plan to write an entire blog post about cesareans and your options in the operating room, but for now I just want to mention a little bit about a “gentle” or “family-centered” cesarean. Making slight changes in a cesarean birth plan can often lead to mothers being happier with their experience, which leads to less chance of postpartum depression. You can read a bit more about these options HERE and HERE. You can also read some real life stories from moms who’ve had cesareans HERE.

While I know there may be many more options and hospital policies to explore, these are the first ones that came to mind. If you have others you’d like me to write about, leave them in a comment below and I will do my best to post about them soon!
I hope this is a helpful article for those of you planning a hospital birth! If you’d like to read more about birth options, you can see the rest of the series below:
